What is MRI?
Key MRI Concepts
•MRI uses magnetic fields to manipulate and image hydrogen atoms in the body.
•Different tissue types are variably influenced by these magnetic fields, resulting in their variable appearances on MRI
•Each MRI sequence (set of images) can emphasize a unique tissue characteristic of the imaged body part
•MRI scanners do NOT use radiation
•MRI studies consist of adjacent, contiguous MRI slices, which overall create a 3-D representation of the imaged body part
•MRI provides excellent soft tissue detail and is commonly used in outpatient and emergency settings
•Most MRI studies take about 20-45 minutes to complete
•Due to the powerful magnetic fields involved, MRI presents unique safety concerns
Editor’s warning: If you were grimacing as you glossed over the physics of X-ray, CT, and ultrasound, the physics of this post will probably make you cry. Frankly, it makes many radiologists a bit weepy. I was lucky to have learned MRI physics from one of the best, Dr. Emanuel Kanal, who teaches national courses to other radiologists. In the intervening decade since he taught me, some of the more esoteric physics details have become a bit…hazy. But don’t worry, radiologists can still expertly interpret MRIs with knowledge of key “practical” MRI physics principles.
What’s in a name?
MRI = Magnetic Resonance Imaging. The full name is nuclear magnetic resonance imaging, but perhaps NMRI was a bit too clumsy for marketing purposes. Let’s briefly examine these words, in no particular order:
- Magnetic: magnets are involved.
- Imaging: pictures too. Check.
- Nuclear: here we are talking about the nucleus of an atom, the part at the center composed of protons and neutrons (nuclei=more than one nucleus).
- Resonance: For better or worse, this is what we will spend the rest of the article explaining, and what ultimately allows MRI technology to work. Resonance refers to the ability of nuclei to both absorb energy in the form of electromagnetic radiation and later release energy back into the environment. That released energy can be detected by MRI machines and used to create images.
Buckle up for MRI physics

As I dive headfirst into details of the physics, I will attempt to walk the line between oversimplification and complete explanation. I want you to understand as much as possible, but these concepts are the stuff of entire textbooks, and I learned merely the basics over an intense weeklong course and five year residency. It would be impossible to cram all that into one blog post.
That said, I can summarize the section on physics in one short sentence:
MRI uses hydrogen atoms to create images.
One of your first questions may be: why hydrogen atoms? Well, they are abundant in water (H2O) and fat, which together account for up to 90% of human body weight. Thus, we can obtain MRI images in almost every part the body.
Hydrogen atoms—the protons in the nuclei, to be more precise—behave like little magnets, with positive and negative poles (google “proton magnetic moment” if you want to know how this occurs, and you will know why I skipped an explanation). An MRI scanner contains a big, powerful magnet. When you lie down inside an MRI scanner, all of the hydrogen atoms in your body flip to align with the scanner’s magnetic field (isn’t that cool? Not to worry, you can’t feel it). This alignment is the first step in creating an MRI image.
For MRI to make sense, we must recognize the relationship between electricity and magnetism. You might use both of these terms to describe your last date, but they are also intimately (see what I did there) related in the field of physics via the concept of electromagnetism. Two aspects of electromagnetism are relevant to MRI:
- Electric current produces a magnetic field: Among other things, this is how the MRI scanner creates its strong magnetic field
- Magnetic fields can create electric voltage: When our tiny hydrogen atom “magnets” flip around, the MRI scanner can actually detect those moving magnetic fields in the form of voltage changes. This constitutes the final step in acquiring an MRI image.
Knockin’ down hydrogen atoms
Imagine a patient is lying inside an MRI scanner with all her hydrogen atoms aligned with a super-strong magnetic field, which we call B0 (B zero). I like to think of this field “Magneto”. I will soon explain how Magneto is created by the scanner, but for now just know it’s there.
To understand this next part, we must dust off the geometry section of our brains and talk about the Cartesian coordinate system. A three-dimensional space can be described by three perpendicular planes: x, y, and z. For MRI physics purposes, the z-axis is aligned parallel to the external magnetic field of the scanner, and thus parallel to our hydrogen atoms (The z-axis is drawn as a vertical line by convention, but remember that in the MRI scanner the z-axis runs parallel to the floor, along a line from the patient’s head to toes).
So our hydrogen atoms in the body are lined up parallel to Magneto. You can think of them as “standing” straight and tall along the z-axis (fig. 1).

What next? We knock him down! How to we do this? We apply another magnetic field, called a radiofrequency (RF) pulse, which I think of as a strong gust of wind. This “gust” lasts but a few milliseconds, until the hydrogen atoms are lying flat on the “ground”, 90 degrees from their previous orientation along the z-axis.

Hydrogen atoms (and the Queen’s guard) don’t take kindly to being knocked down, and as soon as the “gust of wind” subsides, they begin to stand up under the influence of Magneto. In short order, they are back to their original positions, parallel to the z-axis.
Key concept: The MRI scanner can detect the tiny voltage changes that are produced by hydrogen atoms as they stand up again, and use that data to create an image.
Great. Umm, how exactly does that make an image again?
In short, the speed and manner in which the hydrogen atoms get “up” varies among tissue types, and accounts for their variable appearances on MRI.
To help visualize this, let’s revisit Hydrogen Harry from our illustration above, after he has just been knocked down by an RF pulse (fig. 2). The position of his head represents the amount of magnetization of the hydrogen atom. As he slowly gets up, you can imagine two things simultaneously and continuously changing:
- His head moves up until he is standing fully. Over time, this value—called longitudinal magnetization—increases.
- His head moves sideways until it’s back to the “middle”, lined up with the z-axis. Over time, this value—called transverse magnetization—decreases.
The value of #1 for a given tissue is called the T1 relaxation, or simply T1. and that of #2 is called the T2 relaxation, or T2.

As we said, T1 and T2 values differ among different tissue types. So Hydrogen Harry may represent one type of tissue whose hydrogen atoms move slowly up and to the middle, but sprightly young Hydrogen Hannah (a different tissue type) may be quick to move up and to the middle. Other tissue types run the gamut of different T1 and T2 values, but it’s important to emphasize that each tissue type (liver, fat, muscle, etc.) has specific T1 and T2 values that are unchanging.
It’s time for your favorite: a terminology interlude. With CT, we used density to describe the appearance of tissue on an image. MRI measures different characteristics of hydrogen atoms, and detects voltage changes as they move in the magnetic field. You can think of those voltage changes as faint radio signals the MRI scanner can “hear”; thus, when we talk about the appearance of an MRI image, we use the term signal intensity. Increased signal intensity means brighter appearance on the MRI image.
I is for imaging!
I know, I know, I am getting to the image creation part.
You may be wondering how all these fancy tricks with hydrogen and magnets translate into a freaking picture. Well, with our nascent knowledge of T1 and T2, we can begin to understand the basics of how an MRI image is created.
The first concept to understand is that MRI studies are separated into what are called “sequences”—sets of images that represent different views of the body part being imaged. In general, each sequence evaluates one tissue characteristic, such as T1 or T2. We use the term T1-weighted for a sequence that evaluates T1 characteristics in a given body part. While other types of MRI sequences have been devised, T1-weighted and T2-weighted sequences are the workhorses for much of MRI imaging.
Where am I?
Though it may not be obvious, there is a significant piece of information still missing before we can create MRI images: location, location, location. The process of determining the location of an object on MRI is called spatial encoding.
The B0 magnetic field (Magneto) and the subsequent RF pulse (the gust of wind) exert their effects on the entire body part that is being imaged. But in order to create a useful MRI sequence, the radiologists need to see thin slices of that body part, one at a time. Think of an MRI sequence as a loaf of bread with slices of equal thickness (I describe this concept more in my post about CT). Each image corresponds to one slice of bread, and the images together represent an entire 3-D volume of the body part.
Luckily, the geniuses who invented MRI devised a method by which we can “select” a given slice of a body part such that only that exact slice is affected by the RF pulse. This is achieved by applying another magnetic field, using what is called a linear magnetic field gradient along the length of the z-axis.
So we have selected a thin slice of the body. There is still missing information: exactly where the signal originates on the surface of that “slice of bread”. By applying two more linear magnetic field gradients—perpendicular to each other in the x-axis and y-axis—we can encode each small volume of tissue with a specific location. The end result is that our MRI scanner knows exactly where the signal comes from. Isn’t that amazing (and exhausting)?
If you have obtained an MRI, you are certainly familiar with these linear magnetic field gradients. Remember loud banging sounds during the scan? That noise is a result of the electric coils used to create linear magnetic field gradients. As electricity is rapidly turned on and off over several milliseconds, the coils expand and contract slightly, resulting in audible vibrations.
Summary of MRI principles
1. Apply very strong magnetic field (Magneto) to the body. Hydrogen atoms line up.
2. Apply RF pulse (gust of wind) to knock hydrogen atoms down.
3. Apply linear magnetic field gradients in all three planes for spatial encoding. As a result, we are able to localize of the positions of each hydrogen atom.
4. MRI scanner detects the movement of hydrogen atoms as they “stand back up”, and maps them to the appropriate position to create an image slice.
5. Steps 1-4 are repeated multiple times for each slice to create an entire set of images, forming a 3-D picture.
6. Steps 1-5 are repeated separately—with different parameters—to create each unique MRI sequence. Usually 5-10 sequences are needed for a complete study.
The scanner
Shifting gears for a moment, I want to describe the technical marvel that is a modern MRI scanner. If you have ever seen an MRI scanner, it looks remarkably similar to a CT scanner. A donut-shaped structure contains equipment that creates the magnetic fields and detects signal from the patient; the hole in the middle of the donut is called the bore of the magnet. The patient lies on a table which moves into the bore during the MRI scan.

The magnet is always on
In my opinion, the most incredible component of an MRI scanner is the “superconductor” magnet that creates the extremely powerful B0 magnetic field (Magneto), which is hundreds of thousands times stronger than Earth’s magnetic field. How the heck is this accomplished!?
Electricity and magnetism, as we have discussed, are intimately related to each other. MRI machines contain a long cable made from a special combination of metals: niobium-tin encased in copper. When this cable gets really really really cold, it becomes a superconductor, meaning that electricity running through the cable encounters almost no resistance (I will describe why this is important in a minute). MRI scanners keep these cables at -269°C, which is 4 degrees above absolute zero—the coldest temperature possible in the universe! How? It turns out helium is good for something other than balloons and funny voices; liquid helium temperatures hover right around -269°C.
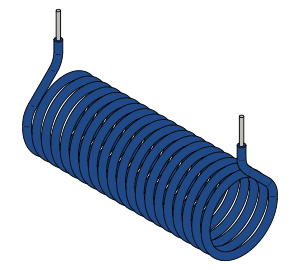
The supercooled, superconducting cables must be oriented in a special configuration (called a solenoid) to create the magnetic field inside the bore of the MRI scanner. A solenoid is like a collapsed slinky or coiled garden hose, with multiple loops of circular cable immediately next to one another. When electric current is run through a cable in this configuration, Magneto is generated in the center (corresponding to the bore of the MRI scanner).
As alluded to in the section title, this powerful magnetic field is always on. One can’t just flip a switch and turn it off. To understand why, we need to talk about how the magnetic field is created during installation of an MRI scanner, a process called “ramping the magnet.” The electric current needed to create such a powerful magnetic field is near 1000 amps—as much as 10 entire modern homes! If hospitals actually had to draw that amount of electricity from the grid for each MRI scanner, it would be cost prohibitive to operate them. So what gives?
Well, we don’t actually keep the MRI plugged in, so to speak—at least not the superconducting magnet part. During installation of the magnet, the current through the supercooled cable is slowly ramped up over 2-3 days until it reaches the desired level of 1000 amps. Then, the ends of the cable are “connected” to each other to create a continuous loop, and current is able to run indefinitely without using any additional electricity. This is what “superconducting” means: the supercooled cables can conduct electricity with essentially no resistance.
The only way the current can be stopped—and the magnetic field turned off—is by heating up the cables back to room temperature, which increases resistance and eventually stops the current. Guess what happens when you heat up liquid helium to room temperature? It becomes helium gas via explosive boiling, called “quenching” the magnet. WE REALLY TRY TO AVOID THIS. It can cause physical damage to the scanner, and the amount of liquid helium needed to cool a scanner costs hundreds or thousands of dollars.
Coils, coils, coils!
Creation of Magneto, our B0 magnetic field, was performed by the superconducting magnet. The remaining steps for MRI image creation are performed by coils, electricity-conducting cables which can also create magnetic fields. Coils come in a couple of different flavors:
- Transmit/receive coils: These coils both create the RF pulse to knock down hydrogen atoms (the transmit part) and listen for the signals from the hydrogen atoms as they stand back up (the receive part). To improve the sensitivity of these coils, especially in relation to receiving signal, coils are manufactured in varying shapes and sizes to conform to the body part being imaged; examples are body, head, or knee coils, to name a few.
- Gradient coils: Critical to spatial encoding (determining location within the body part), these coils are mounted inside the bore of the magnet, closer to the patient than the superconducting magnet. As noted above, these buggers are responsible for the loud knocking sounds you hear during an MRI scan.
I’m special, so special
While T1 and T2 are the most common MRI sequences, a few other “special” sequences are important, interesting, or both. This list is by no means exhaustive, but rather a taste of the flexibility and creativity that is possible when devising MRI sequences.
- Proton density: As the name implies, a proton density sequence simply measures the number of protons occupying each area in the imaged body part. This sequence is obtained similarly to T1 and T2 sequences, with slightly different parameters. It is particularly useful in musculoskeletal imaging; more specifically, it is an important sequence in looking for meniscus tears on knee MRI
- Diffusion-weighted imaging: This unusual sequence looks at the movement of water molecules. When water molecules are not able to diffuse (move around) freely, they stand out as bright areas on a diffusion-weighted image, so obvious that your blind Uncle Charley could see them. Tissues that are damaged tend to accumulate fluid, trap water molecules, and thus show up as bright spots on these sequences. Diffusion-weighted imaging is most frequently used in the brain to look for stroke.
- Fat suppression: In the midst of the holiday season, we all could use a little fat suppression. Alas, these sequences do nothing to melt away cookie-induced blubber, but rather work to decrease the signal of (i.e. darken) fat on a given MRI sequence. Two major techniques—called inversion recovery and chemical fat saturation—are used to accomplish suppression of fat signal; the details of these techniques are complicated and not important, but just understand that it makes fat darker. Why is dark fat sometimes useful? Normal fat is bright, and can hide important abnormalities, especially areas of fluid or edema. When we suppress the signal from fat, it makes these abnormalities really stand out. Fat suppression can be used on different types of sequences, including T1 and T2.
- Post-contrast: Critical information can sometimes be obtained by injecting intravenous contrast (dye) before an imaging sequence. These contrast agents use compounds containing the element gadolinium, which exerts a small magnetic effect on adjacent tissues. As a result, tissues that preferentially take up contrast appear brighter on T1 sequences.

Assault with a deadly floor buffer
I’ll begin this section on MRI safety with a legendary story from my residency training. Installation of a new MRI scanner had run into late evening, and the individuals installing it went home to continue work the next day. No one knows exactly what occurred that night, but signs warning a powerful magnetic field was present were either not displayed correctly or not seen by the individual cleaning the floors. When this unsuspecting janitor waltzed into the room—I like to picture him rocking out with headphones on—his large metal industrial floor buffer first began to levitate, then rocketed into the bore of the MRI at incredibly high speed. Despite everyone’s best efforts—which included attaching a winch to the door frame, and subsequently ripping off that frame—the floor buffer could not be extracted from the magnet. The attraction of the metal in the buffer was simple too strong to counteract, and the magnet had to quenched at great expense.
I hope this cautionary tale illustrates the power and potential peril of MRI scanners, given the incredible strength of the B0 magnetic field. MRI magnets are just like other magnets: they attract metal. The technical term for a material that is attracted by magnetic fields is ferromagnetic. Any medical equipment or other object that may be ferromagnetic must be carefully excluded from the room containing the MRI scanner, lest they become unintentional missiles. On more than one occasion, oxygen tanks have inadvertently entered the MRI room and become airborne at very high speeds, injuring or even killing patients. These are fortunately extremely rare occurrences.
Pieces of metal located in a patient’s body also bear special attention. These objects include surgically placed metal plates and screws as well as bullet fragments or other shrapnel. Hopefully patients know about these metal objects, but sometimes there is a “surprise” bullet or two that had been forgotten. If there is any doubt about the presence of metal, X-rays are first obtained of the body part in question to look for it.
Metal in the body can be hazardous in two ways: it can move, and it can heat up. If metal is located in certain parts of the body—near the eyes or brain, for example—the risk of injury precludes getting an MRI. Much of the time, the patient can undergo MRI with appropriate precautions, meaning they are instructed to immediately tell the MRI technologist if they experience any heating or discomfort near the metal.
Cardiac pacemakers and other implanted devices also deserve special attention during an MRI scan. RF pulses and gradient magnetic fields can create a current in the wires of these devices, heating them up to a degree that skin burns can occur. The powerful B0 magnetic field can also cause certain programmable implants to malfunction during the scan, not something you want to happen with a pacemaker. The safety of these devices varies by type and manufacturer, and is always checked by the MRI technologist prior to scanning.
For these reasons, each patient undergoes extensive safety screening—far beyond what I have discussed here—before they step anywhere near an MRI scanner.
What can we image with MRI?
The real question is: what can’t we image?
MRI is excellent at providing detailed imaging of soft tissues in all parts of the body, both in outpatient and emergency settings. An important consideration when choosing MRI is time: MRI scans take anywhere from ~20-45 minutes, much longer than a several-minute CT scan.
Some common uses of MRI include:
- Head: stroke, brain tumors, and many other brain abnormalities
- Spine: evaluate back pain
- Abdomen and Pelvis: evaluate abdominal pain and other abnormalities, especially related to the biliary system. Male and female pelvic organs are seen well with MRI.
- Bone: evaluate pain or infection in bones and joints.
- Breast: identify and characterize breast cancer
Uncle!
Believe it or not, I barely scratched the surface on many of these topics. Honestly, this post could have been three times longer, still leaving great deal out. For example, you might have noticed I glossed over the visual appearance of MRI images, and why each tissue type looks a certain way on a given sequence. Perhaps another day, in another post. Regardless, I hope you enjoyed the whirlwind tour of MRI.
I wouldn’t be surprised if you have questions or comments, so please post them below!
